COVID-19 has had a profound impact on our daily lives. The novel coronavirus changed the way we go to work, buy groceries, and interact with our friends and families. At Response Biomedical, we’re also very aware of how the virus has illustrated the strengths and limitations of rapid diagnostics.
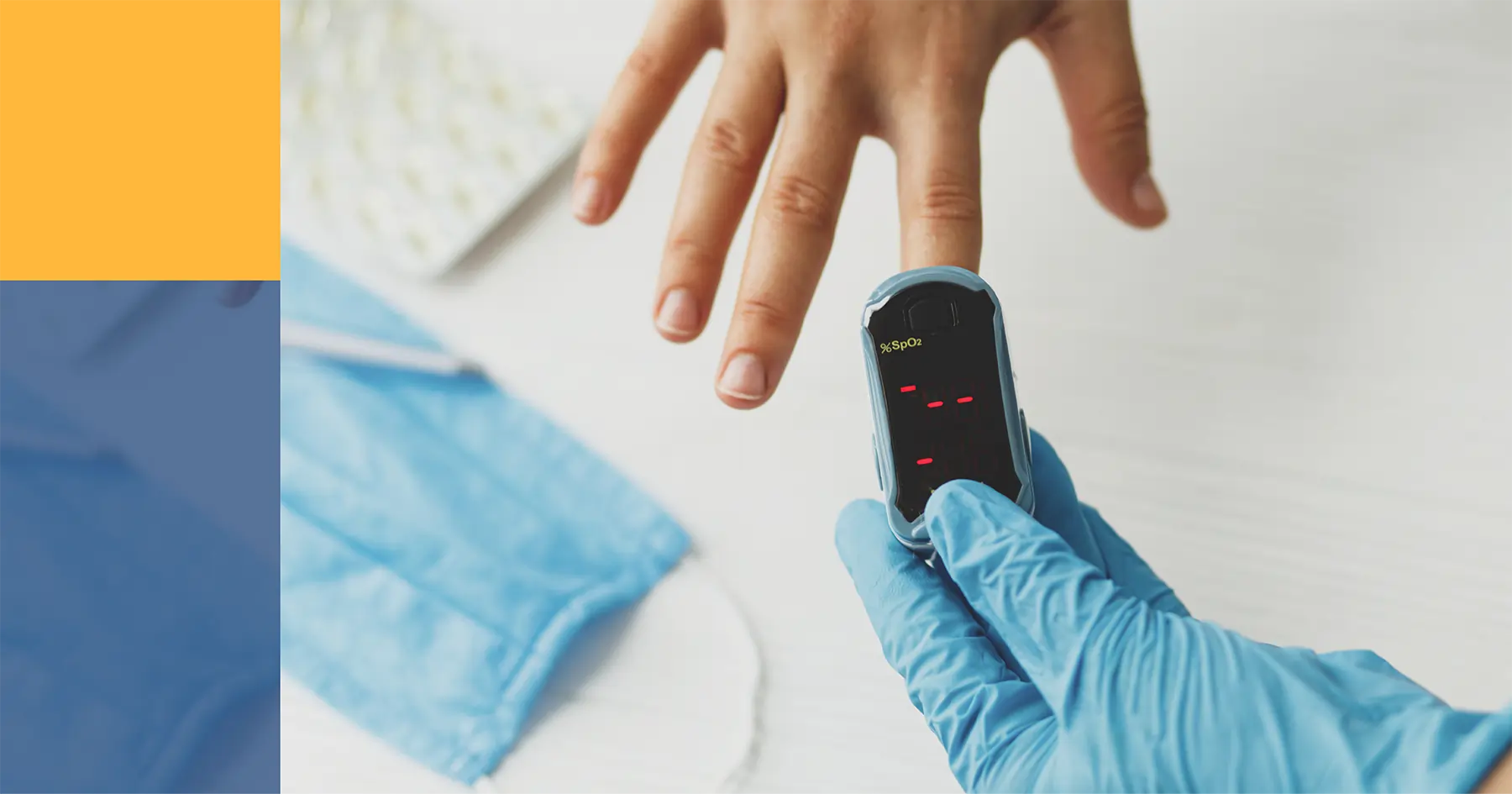
Point of Care (POC) testing is defined as medical diagnostic testing at or near the patient, at the time and place that testing is required. Although many hospitals had previously implemented POC platforms, before the COVID-19 pandemic began, rapid testing rarely made national headlines. Now, rapid testing has increasingly become part of the effort to slow the spread of COVID-19.
With the implementation of 15-minute COVID-19 point-of-care tests in hospitals, medical clinics, and pop-up test centres, rapid tests are being used at an unprecedented rate. With the increased attention, we’re seeing more studies and opinions on the benefits and challenges of POC.
In the article below, we’ll look at what rapid tests bring to the healthcare system. We’ll also discuss how medical staff can take advantage of POC testing during the ongoing fight against COVID-19 and beyond.
How COVID-19 Ushered Rapid Testing to the Mainstream
The SARS-CoV-2 pandemic’s spread is an ongoing global drama. According to the latest totals, there have been 169 million cases and over 3.5 million deaths, as of May 28, 2021. But since early 2020, the World Health Organization has made one thing very clear — to keep the spread of the novel virus to a minimum, nations must “test, test, test.”
In early 2020, countries around the world began manufacturing rapid testing kits, the goal of which was to detect the presence of the virus without putting undue strain on testing laboratories. Rapid and reliable detection of the virus allows healthcare providers to isolate those who are infected quickly and administer treatment.
Rapid testing isn’t a new way to identify viral infections. A study in 2018, for example, found that fast turnaround time and relative accuracy of POC testing could “lead to more appropriate prescription of treatments for infectious agents.” What made rapid testing so vital to the COVID pandemic, however, was the very real danger of asymptomatic carriers unknowingly spreading the virus.
It’s worth noting that even with the advent of COVID-19 vaccines, rapid testing will still play a vital role in the safety of the public. For many on the frontlines, there’s little doubt that point-of-care testing has helped them save the lives of the most vulnerable.
Point of care testing enabled us to be responsive and effective against Covid to keep those in our care staff. It allayed the fears of so many too.
— Anita Peet MBE 💚 (@PeetAnita) April 22, 2021
Challenges of Modern Point of Care (POC) Testing
When dealing with dangerous, highly transmissible diseases, accuracy must go hand-in-hand with affordability. Even if the reagents and platforms are widely available and cheap enough to deploy across a healthcare system, they must provide data that medical professionals can trust.
False positives and false negatives happen for a number of reasons. In November 2020, once POC antigen tests had begun saturating health sectors, the U.S. Food and Drug Administration released a disclaimer warning medical staff that rapid COVID tests can produce inaccurate data. They gave multiple reasons for the results:
- Improper handling of the test card or packet
- Batch testing can distort incubation time
- Insufficient cleaning resulting in cross-contamination
- Reading results before or after the designated time
The FDA also notes to always consider the medical history and clinical observations of the patient. When a rapid antigen test gives information you feel is inadequate, medical staff should follow it up with the gold standard reverse transcription-polymerase chain reaction (RT-PCR) test.
1/ Highly sensitive, rapid point-of-care #Covid19 testing is ideal. Unfortunately, we currently have no such test. @michaelmina_lab saying otherwise is magical thinking.
— Bob Darnell (@darnelr) February 6, 2021
Let me explain why.
Training: A Key Concern with Point-of-Care Tests
While test sensitivity is an obvious concern for medical staff, adequate training underlies much of what the FDA mentions above. It’s true that there are no standard training practices for rapid tests, so instructions can vary from one rapid test to another.
A recent article in Nature magazine pointed out that manufacturers are also more likely to follow the proper training methods during their clinical trials, which doesn’t always work in the real world.
When we think about POC tests in homes, schools, or restaurants, how the tester holds the swab or how long they wait before adding the material to a test card can greatly affect the results. This isn’t just a challenge today, but one that will become an ongoing issue with the prevalence of rapid tests being used by the public.
In a medRxiv preprint study, researchers found that sensitivity reached only 58% with at-home testers using assays, while laboratory scientists using the same assays reached almost 80% sensitivity.
New Opportunities for Point-of-Care Testing
COVID-19 has given more hospitals across the country a reason to install rapid testing platforms, and that opens the door to a clear opportunity for other tests to be performed on the same machines.
We've completed almost 10,000 COVID-19 tests using rapid point-of-care testing systems since beginning clinical pilots in December.
— Tyler Shandro (@shandro) January 14, 2021
The broader implementation of rapid testing is now underway in all AHS zones. 1/3 #abhealth #ableg #COVID19AB
But for POC tests to be as accurate as possible, medical facilities must create and follow standards and practices. In HealthcareTransformers, Dr. Tony Cambridge notes that a decentralized testing program could relieve the pressure facing the UK’s National Healthcare System.
Getting test results fast means there are fewer hospital beds filled with patients waiting 24 hours or more for a result. Dr. Cambridge goes on to note that effective POCT services must have a clear managerial structure, which includes:
- Standardized devices
- Training and competency
- Documentation
With Response Biomedical’s latest RAMP platform, we offer digital results and 24/7 world-class support. The system can perform up to 6 independent tests per machine without any warm-up time or calibration requirements. This allows trained medical staff to relieve the stress facing their laboratories, and to run a variety of different diagnostic tests on a single device.
The Future of Point-of-Care Testing Is Bright
When the COVID-19 pandemic finally subsides, one thing will remain clear: rapid testing is here to stay. By maintaining adequate training practices and keeping medical staff up to date, POC systems will continue to save lives and reduce needless medical costs.
If you’re interested in learning how you can make accurate and fast patient care decisions with our rapid testing and acute care diagnostic solutions, contact us today.