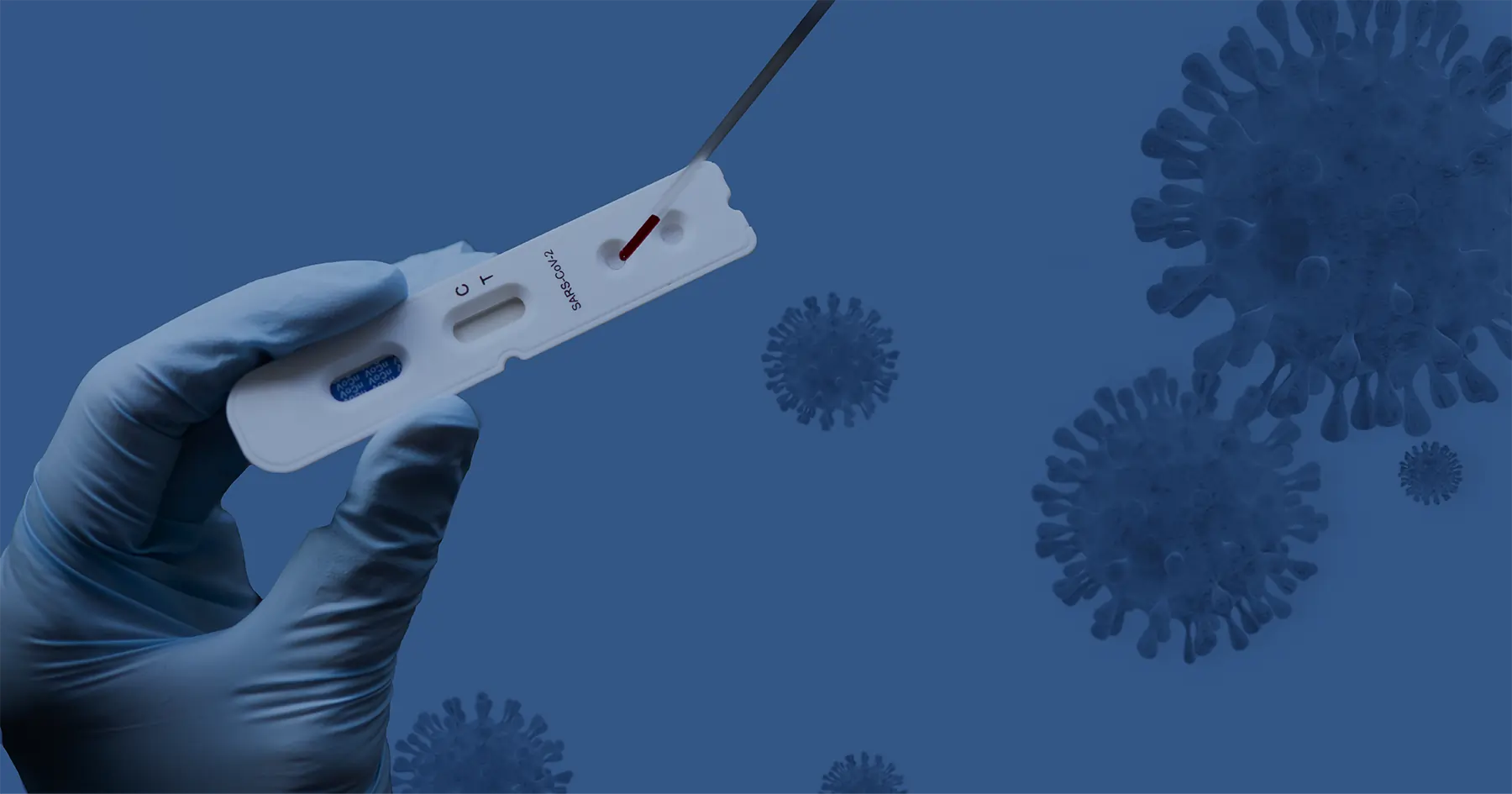
This past year, rapid testing solutions became infamous because of the crucial role they play in detecting COVID-19. The epidemic has shown first-hand just how important real-time results are in making informed healthcare decisions and improving patient well-being. But what is rapid testing and how can medical staff use it in their everyday interactions with patients?
In the guide below, we’ll tell you everything you need to know about rapid testing. This includes what it is, why it’s important, and how it can help healthcare providers improve their ability to diagnose and treat chronic illnesses and acute health issues.
In this guide:
What Are Rapid Testing Diagnostic Tests?
Rapid testing is a type of health diagnostic tool that physicians and medical staff use to get real-time results within minutes. These tests can be performed near the patient or at the point of care (POC) with minimal training and upkeep.
There are various types of rapid tests available in the market. Some rapid tests, such as lateral flow assays or dipsticks, have been around for decades. Some of these tests can even be purchased over the counter such as pregnancy tests.
Other point-of-care (POC) tests harness advanced technology and require a desktop instrument or “analyzer” to read the results. These analyzers can even provide the capability to store and transmit the results digitally to physicians or specialists for analysis and interpretation.
How Does Rapid Testing Work?
The main goal of point-of-care testing is to safely and securely collect a specimen, test it, and generate results at the bedside or within close proximity to the patient. That way, physicians can quickly begin a treatment plan while the patient is still with them. POC tests can give a physician critical patient insights without the need for a traditional laboratory.
Rapid tests often require a blood or urine sample from the patient or person being tested. The sample is then processed to detect a specific molecule called a biomarker (short for biological marker) which is the target of the given test. The results can be delivered in a qualitative, quantitative, or semi-quantitative format.
- Qualitative results typically will show a positive or a negative result that is not numerical such as that seen with a rapid visual pregnancy test.
- Quantitative will show a numerical result that corresponds to the amount of the biomarker in the blood: these types of tests are needed to measure more accurately the concentration of something in the blood such as glucose monitoring or tracking of a biomarker that indicates a disease condition at a certain level.
- Semi-quantitative tests are in the middle of the two, and may offer a rough estimate of how much of a given biomarker is present, without necessarily giving a number.
Depending on the method used for interpreting the result, a rapid test can be a visual test or may require an analyzer to read the result. With desktop and handheld analyzers, the patient sample is mixed with the appropriate reagent, placed on the test cassette, then inserted into the test port. Within two to thirty minutes, the analyzer will detect the cassette, identify the specific biomarker and provide a result.
Types of Rapid Testing Devices
Rapid testing devices fall into three categories, which are:
Desktop Diagnostics: Devices, such as the RAMP systems, installed in clinics, pharmacies, and hospitals. They are self-calibrating and offer lab-quality accuracy.
Hand-Held Analyzers: Palm-sized devices that can be brought to the bedside.
Strips: Commonly available over the counter. Urine dipsticks or pregnancy tests are examples of this category.
How Accurate Is Rapid Testing?
Since the 1980s, the technology behind rapid tests has evolved at a fast pace with results becoming more accurate and testing becoming more widely available. In some cases, POC tests can now use lab-based methods when it comes to accuracy depending on the specific test.
But rapid testing accuracy depends on a number of variables. Many such variables stem from the quality of training for the staff on how to administer a rapid test.
The College of American Pathologists offers some examples of what can affect rapid testing accuracy:
- Lack of internal guidelines
- No formal training on the test procedures
- No place to document results
- Failure to calibrate the diagnostic device
- How the sample is collected
- Extreme temperature fluctuations
Benefits of Rapid Testing
Laboratory equipment usually requires high upkeep and is costly to maintain. By limiting the reliance on laboratory testing, POC tests allow for faster turnaround time, improving actionable results.
POC testing can also potentially help improve patient outcomes. By allowing the screening process to be completed in one sitting, physicians are provided with actionable results and may be able to provide options right away.
Within third-world populations, rapid, reliable, and inexpensive POC tests can aid in diagnosing deadly infections. Without these tests, some countries may not be able to afford accurate and reliable data9.
But that’s not all. According to Medical Laboratory Observer, some of the other key benefits of rapid testing are:
- Fast diagnostic turnaround results
- Less reliance on specimen transport
- Reduced blood specimen volume
- Wireless data transmission
- Fewer administrational errors
- More patient-centred care options
- Lower operational cost
What Makes a Good Rapid Testing Device?
With technological advances and the industry-wide desire to improve patient care, physicians are finding more and more reasons to turn to rapid testing. But with the proliferation of brands and products, how can you tell the difference between a poor testing device and a good one?
According to the World Health Organization, the key characteristics of any good rapid testing device are:
- Cost-effective for physicians and patients
- Provide few false negatives and positives
- Easy to use and teach
- Fast results with minimal refrigeration
- Zero need for complicated equipment
- Compact, durable, and sturdy
Rapid Testing and COVID-19
The most prominent recent example of a rapid test is the COVID-19 antigen diagnostic test. Antigen tests have been used to diagnose respiratory pathogens, such as influenza, for years. Rapid COVID-19 tests require a sample from the nose or mouth to detect the presence of SARS-CoV-2 antigens.
COVID-19 antigen rapid tests cost a fraction of the lab-based polymerase chain reaction tests (PCR). One recent study found that antigen-based POC tests were especially helpful in decreasing turnaround time in outpatient settings that were previously experiencing a three-day delay in results with PCR.
Furthermore, the CDC has suggested using antigen tests as a control measure in congregate settings, where prompt results can help control the spread. It’s important to note that potential cases discovered with a COVID-19 rapid test are further identified with a PCR to confirm the viral infection.
Rapid Testing Saves Lives
When every minute counts, you need lab-quality results you can trust. At Response Biomedical, we’re global leaders in medical testing and device manufacturing. Physicians across the world rely on our rapid testing devices to improve patient health.
To learn how you can make faster and more accurate patient care decisions with our rapid testing and acute care diagnostic solutions, contact us today.